DIABETES
We have an intricate knowledge of the effects both type 1 and type 2 diabetes has on your foot health. The two main systems effected by diabetes mellitus are the vascular (blood) system and neurological (nerve) system. Below is some information on signs, symptoms & risks to be aware of as well as advice as to how you and your podiatrist can maintain your feet at their optimal level for as long as possible. You should see a podiatrist at least once a year to undertake cursory neurological and vascular assessment. Routine care which involves nail and skin management is recommended on a 6 to 8 weekly basis.
Heightened blood sugar levels can lead to Peripheral Vascular Disease (PVD).This involves damage to the large arteries of the leg that supply blood to the foot as well as the smaller vessels called capillaries which provide blood to the toes. This leads to an overall reduction in the circulation of arterial blood to the feet.
- feet always feel cold
- skin appears flaky and fragile
- nails acquire a clubbed appearance (rounded surface)
- toenail growth reduced
- breaks in skin take longer to heal
- easily infected following break in skin
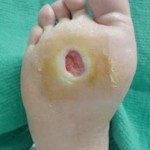
- ulceration
- gangrene
- regularly cut nails and debride callus for client reducing the chance of laceration during self care
- skin care advice
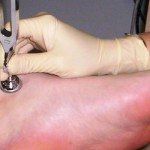
- cursory vascular tests: testing tissue perfusion (temperature of skin) and Subpapillary Venous Plexus Filling Time
- Bidop bi-directional Doppler to monitor circulation within the Dorsalis Pedis & Posterior Tibial arteries
- send annual report of vascular status to your GP or specialist
- feet feel numb
- prone to blistering following undetected pressure from footwear
- prone to ulceration following undetected pressure from footwear
- prone to undetected laceration, puncture or burns to skin whilst walking barefooted
- increased risk of infection following undressed wounds the client is unaware of
- amputation following osteomyelitis
- osteomyelitis following infection from undressed wound
- regular debridement of callus accumulated from undetected stresses
- regular assessment of foot for any change in skin integrity via laceration, puncture or burn
- neuropathic foot care tips e.g. never walk with bare feet, check bottom surface of feet daily
- cursory neurological testing; monofilament, tunning fork, reflex hammer, proprioceptive testing
- send annual report of neurological foot status to GP or specialist